What is Allergic Conjunctivitis?
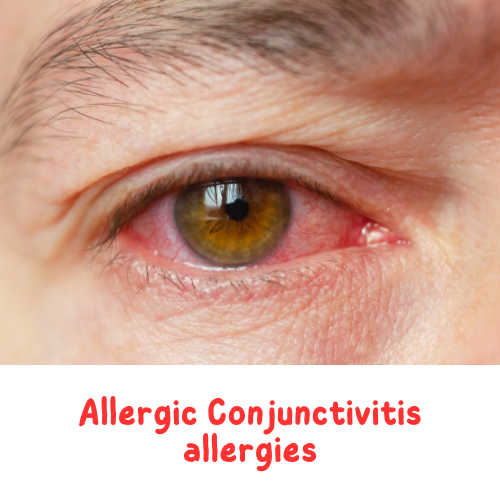

Allergic conjunctivitis is an inflammatory condition of the conjunctiva, which is the thin, clear tissue that covers the front surface of the eye and the inner surface of the eyelids. It occurs as a result of an allergic reaction to substances that are irritants and to allergens, such as pollen, dust, or mold.
In the United States, an estimated 20 percent of the population suffers from eye allergies.
The eyes are an easy target for allergens and irritants for the following reasons:
- Exposure: The eyes are constantly exposed to the external environment, making them susceptible to various allergens and irritants. Pollen, dust, mold spores, pet dander, and other airborne particles can come into direct contact with the eyes. Additionally, certain irritants such as smoke, chemicals, and pollutants can also reach the eyes easily.
- Sensitivity: The eyes are highly sensitive organs. They contain a rich network of nerve endings and are densely supplied with blood vessels. This sensitivity makes the eyes more vulnerable to irritation and allergic reactions.
- Thin and Transparent Tissue: The conjunctiva, the thin, transparent tissue that covers the front surface of the eye and lines the inner surface of the eyelids, is particularly susceptible to allergens and irritants. This tissue is designed to protect the eye and provide lubrication. However, its delicate nature allows allergens and irritants to penetrate easily, leading to allergic conjunctivitis or other forms of eye irritation.
- Rapid Response: When allergens or irritants come into contact with the eyes, the immune system quickly responds to protect the eye from potential harm. Mast cells, a type of immune cell, are present in the conjunctiva and release histamine and other inflammatory substances in response to allergens or irritants. This immune response triggers various symptoms, such as itching, redness, swelling, and increased tear production.
There are two types of allergic conjunctivitis:
Seasonal allergic conjunctivitis: The seasonal form is associated with seasonal allergies that usually occur during the spring and summer months, and sometimes during the fall. Exposure to pollen, grass and other airborne allergens causes seasonal allergic conjunctivitis.
Perennial allergic conjunctivitis: The perennial form persists throughout the year, and is generally triggered by indoor allergens such as animal dander, dust, and mold spores.
What causes the allergic conjunctivitis?
When an individual with a predisposition to allergies comes into contact with an allergen, such as pollen, the immune system recognizes it as a threat. This recognition triggers the release of histamine and other inflammatory substances by specialized immune cells, such as the mast cells in the conjunctiva.
Histamine causes dilation of blood vessels and stimulation of nerve endings in the eyes, leading to the classic symptoms of redness, itching, tearing, swelling of the conjunctiva, and a gritty or burning sensation in the eyes. Some individuals may also experience blurred vision, sensitivity to light, or a watery discharge.
What you can do to minimize your symptoms
The first step is to minimize exposure to allergens. Stay indoors during peak pollen times, typically in the morning and early evening, and keep windows closed to prevent pollen from entering your home. In addition, wearing sunglasses and a hat when outdoors can offer some protection by reducing direct contact with allergens.
Maintaining a clean environment is crucial. Regularly vacuuming carpets, dusting surfaces, and using hypoallergenic bedding can help reduce allergen accumulation. Wash your hands frequently and avoid rubbing your eyes to prevent further irritation and allergen spread.
Over-the-counter saline eye drops or artificial tears can provide temporary relief by rinsing out allergens and soothing the eyes. These drops do not contain medications but can help alleviate itching and discomfort.
For more severe symptoms or inadequate relief from over-the-counter remedies, there are prescription-strength eye drops containing antihistamines, mast cell stabilizers, or non-steroidal anti-inflammatory drugs (NSAIDs) to manage inflammation and relieve symptoms. Allergy immunotherapy, such as allergy shots or sublingual tablets, may be considered for long-term management. Nasal corticosteroid sprays may also be prescribed if you also have accompanying nasal symptoms.
Gregory Scimeca, M.D.
Ophthalmologist and Medical Director
The Eye Professionals
Our Locations
