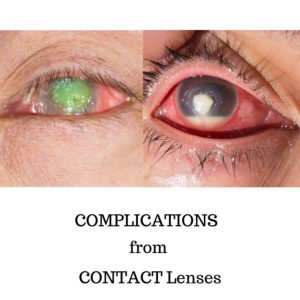
Complications of Contact Lenses

A common complaint of contact lens wear is eye dryness. Dry eyes can be caused by a lack of tear film, oxygen deprivation, lens deposits, or contact lens solution.
Treatment can be as simple as using artificial tears, but sometimes the problem is blepharitis, which is an inflammation of the eyelids.
Treatment for blepharitis is to keep the lids clean, use warm compresses, and clean the eyelids with a mixture of water and baby shampoo. This eye care routine may need to be continually maintained since blepharitis rarely goes away completely. Your doctor can help you find the right treatment for your eye dryness.
Meibomian gland dysfunction is another cause of eye dryness. If your eyes are red and itchy and there is a gritty feeling or the sensation of something in your eye, it could be meibomian gland dysfunction.
The meibomian glands secrete oils onto the surface of the eye and these oils keep your tears from evaporating too quickly. There are several therapies your eye doctor can try that can restore meibomian gland function such as intense pulsed light, lid debridement, and antibacterial or cyclosporine eye drops.
Protein buildup on contact lenses can cause blurred vision and discomfort. Proper handling of contact lenses and using an enzymatic cleaner on your lenses can eliminate protein deposits.
For contact lens users who have continued problems with protein buildup, daily disposable lenses may be the solution to the problem. The longer lenses are used, the greater the risk of protein buildup and infection to the cornea which can damage eye tissue. Eye drops can also help. They not only remoisturize your contacts, but eyedrops made for contact lenses can remove protein buildup. Your eye doctor can help you find the best way to manage excessive protein buildup.
Corneal neovascularization, which is the growth of new blood vessels into corneal tissue from oxygen deprivation, is another contact lens complication. Your corneas need oxygen to stay healthy and contact lenses that have low oxygen transmissibility starve the cornea of oxygen which can lead to the creation of extra blood capillaries that form to satisfy the oxygen demand of your corneas.
Corneal neovascularization can be mild to severe. The first step to correct corneal neovascularization is to stop contact lens wear until the corneal neovascularization can be assessed by a physician and proper treatment started.
Microbial keratitis can also affect contact lens wearers. It is an infection of the cornea that can be caused by wearing contact lenses overnight, not disinfecting the lenses properly, storing or rinsing contact lenses in water, or showering or using a hot tub while wearing contacts.
Microbial keratitis is a sight threatening infection and must be treated promptly. Symptoms are pain, excessive tearing, red eyes, and light sensitivity. Microbial keratitis has different treatments depending on whether it is bacterial or viral. Your eye doctor will have you make follow-up visits during treatment so the keratitis and condition of your corneas can be closely monitored.
Following these recommendations will reduce your risk of contact lens complications:
- Each time you remove your contact lenses, rub and rinse your contact lenses with contact lens disinfecting solution, never water or saliva.
- Never store your contact lenses in water.
- Replace your contact lenses as often as recommended by your eye doctor.
- Rub and rinse your contact lens case with contact lens solution, never water, and store upside down with the caps off.
- Replace your contact lens case every three months.
- Always use fresh contact lens disinfecting solution and never mix fresh solution with old solution.
- Only use the contact lens solution recommended by your eye doctor.


